In the “dry” (atrophic) type of age-related macular degeneration (AMD), deterioration of the retina is associated with the formation of small yellow deposits, known as drusen, under the macula, as shown in the illustration below. This phenomenon leads to a thinning and drying out of the macula, causing the macula to lose its function (4). The amount of central vision loss is directly related to the location and amount of retinal thinning caused by the drusen.
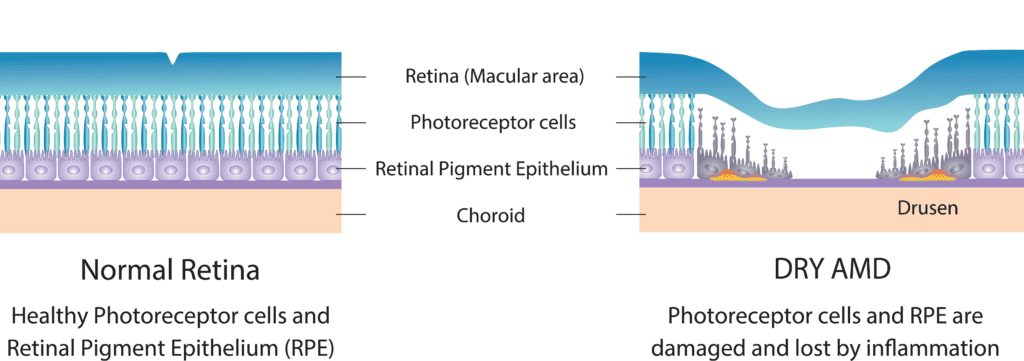
The early stage of dry age-related macular degeneration is associated with minimal visual impairment and is characterized by drusen and pigmentary abnormalities in the macula (5). Drusen are accumulations of acellular, amorphous debris subjacent to the basement membrane of the retinal pigment epithelium (6). Nearly all people over the age of 50 years have at least one small druse in one or both eyes (7). Only eyes with large drusen are at risk for late age-related macular degeneration (8).
This form of macular degeneration is much more common than the “wet” type of macular degeneration, and it tends to progress more slowly than the “wet” type. However, a certain percentage of the “dry” type of macular degeneration turns to “wet” with the passage of time. There is no known cure for the “dry” type of macular degeneration.
Why is it Called ‘Dry’ Macular Degeneration?
There are two basic types of age-related macular degeneration; ‘dry’ and ‘wet’. “Dry” age-related macular degeneration does not involve any leakage of blood or serum, as opposed to “wet” AMD.
Symptoms of Dry Macular Degeneration
Patients with this “dry” form may have good central vision (20/40 or better) but substantial functional limitations, including fluctuating vision, difficulty reading because of their limited area of central vision, limited vision at night or under conditions of reduced illumination (2 & 3).
What the Patient may see:

Center vision may appear blurry because parts of the macula have begun to die, leaving blank spots in vision. Straight lines may look wavy. Side or “peripheral” vision is rarely affected.
Click here for a video showing what a person with macular degeneration sees.
Prevalence of Dry Macular Degeneration
Approximately 85% to 90% of the cases of macular degeneration are the “dry” (atrophic) type.(1.)
Treatments for Dry Macular Degeneration
The treatment for early dry AMD is generally nutritional therapy, with a healthy diet high in antioxidants to support the cells of the macula.
If AMD is further advanced but still dry, supplements are prescribed, to add higher quantities of certain vitamins and minerals which may increase healthy pigments and support cell structure.
References
1. JM Seddon, Epidemiology of age-related macular degeneration. (AP Schachat, S Ryan eds.) Retina, 3rd ed. St. Louis, MO: Mosby; 2001;1039-50.
2. JS Sunness, Visual function abnormalities and prognosis in eyes with age-related geographic atrophy of the macula and good visual acuity. Ophthalmology. 1997;104:1677-91.
3. RL Steinmetz, Symptomatic abnormalities of dark adaption in patients with age-related Bruch’s membrane change. Br J Ophthalmology. 1993;77:549-54.
4. S Parmet, Age-related macular degeneration. JAMA. Vol. 288 No. 18. 2001;2358.
5. AC Bird et al, An international classification and grading system for age-related maculopathy and age-related macular degeneration. Surv Ophthalmol 1995;39:367-74.
6. NM Bressler et al, Clinicopathological correlation of drusen and retinal pigment epithelial abnormalities in age-related macular degeneration. Retina. 1994;14:130-42.
7. R Klein et al, Prevalence of age-related maculopathy: the Beaver Dam Study. Ophthalmology. 1992;99:933-45.
8. R Klein, The five-year incidence and progression of age-related maculopathy: the Beaver Dam Eye Study. Ophthalmology. 1997;104:7-21.

