Geographic Atrophy (GA), is an advanced form of dry age-related macular degeneration (AMD) that causes cell death (atrophy) in areas of the retina and can lead to irreversible vision loss. It is characterized by large, well-demarcated sections of the retina that stop functioning.
A diagnosis of GA must be made by an eye care specialist, based on images taken of the eye.
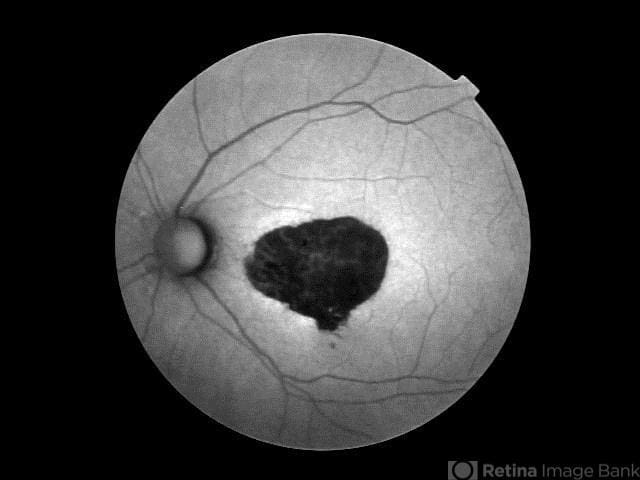
Fundus autofluorescence of geographic atrophy
This image was originally published in the Retina Image Bank® website. Photographer: Mitzy E. Torres Soriano, MD; Centro medico Cagua-Estado Aragua. Venezuela. Retina Image Bank. 2015; Image Number 24990. © The American Society of Retina Specialists.
In GA, the areas of atrophy have clear borders, as seen in the image above. Each defined area of atrophy is called a lesion. As lesions develop, aspects of visual performance can be diminished, such as reading, driving, and seeing in low light. As the lesions expand, and sometimes overlap, they begin to grow into and affect the fovea (the center of the macula, responsible for sharp vision), causing blind spots (scotomas) and loss of visual acuity in central vision.
GA can occur late in the progression of “dry” AMD, and can also occur even after “wet” AMD has developed and after the use of anti-VEGF injections to stop “wet” AMD. Patients with GA can also develop “wet” AMD.
Why is it called “Geographic Atrophy”?
In images of the retina, areas of dead cells (atrophy) resemble a map, hence the term “Geographic Atrophy.”
Symptoms of Geographic Atrophy
Many of the symptoms documented for Geographic Atrophy are the same, or overlap with Dry AMD, so symptoms alone are not the best indicator of Geographic Atrophy, but can include:
- Difficulty adapting to low light levels
- Need for brighter light
- Images appear with decreased intensity of brightness
- Reduced central vision
- Blurriness of printed words
- Visual distortions
- Difficulty in recognizing faces
Prevalence of Geographic Atrophy
- GA accounts for 20% of all legal blindness attributed to AMD
- Affects approximately 1 million people in the United States
- Affects approximately 5 million people worldwide
- Starting at age 50, prevalence quadruples every 10 years, from 0.16% at age 60, to 2.91% at age 80
What are the Chances that Dry AMD will Develop into Geographic Atrophy?
30% of Dry AMD patients will progress to geographic atrophy.
Risk of developing GA increases as dry AMD advances from early to intermediate, with age, and there is some evidence that risk of GA also increases with certain risk factors such as:
- Smoking or a history of smoking
- Lens opacities
- Previous cataract surgery
One of the strongest risk factors is poor visual acuity at baseline. A study found that patients with visual acuity at or worse than 20/200 had almost a 3-fold greater risk of developing GA than those with a baseline of 20/25-20/40.1
Additionally, several chronic conditions are associated with increased risk of AMD progression. Managing any chronic medical condition should be part of your overall AMD management to reduce the risk or rate of progression of AMD and the potential development of geographic atrophy.
- Obesity
- Cardiovascular disease
- Diabetes
- High cholesterol
What are the Chances that a Wet AMD patient will also Develop Geographic Atrophy?
Up to 37% of wet AMD patients can develop geographic atrophy within 2 years. That risk increases over time, so by 7.3 years, 98% of patients with wet AMD can also develop geographic atrophy.
Who Should be Examined for Geographic Atrophy?
If you have a family history of AMD, you should work with an eye care specialist to establish a routine of thorough eye exams. At 40, it is recommended that everyone have a complete, dilated pupil eye exam to establish a baseline for eye health.
While currently there are no medically established guidelines for the frequency of eye exams between the ages 40-60, if there is a history of AMD in your family, the American Macular Degeneration Foundation suggests regular exams during that time frame. Early detection can lead to early intervention, a slowing of disease progression, and the preservation of useful sight.
Between 60-65, you should have a dilated pupil eye exam at least once a year, and possibly every 6 months.
If you have been diagnosed with dry AMD, you should have a dilated pupil eye exam at least once a year, every 6 months, or more often if suggested by your retina specialist..
In addition to a family history of AMD, the following risk factors may contribute to the development or progression of GA:
- Smoking or history of smoking
- Obesity
- Cardiovascular disease
- Sleep Apnea
- Poor diet
- Diabetes
- High Cholesterol
- Long-term use of calcium-channel blockers (see: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9296271/)
How is Geographic Atrophy Diagnosed?
Clinical Diagnosis
Geographic atrophy is a clinical diagnosis, meaning the diagnosis is made by your eye doctor based on your symptoms and what they can see using diagnostic imaging.
Diagnostic Imaging
- Fundus autofluorescence – currently the standard imaging technology to visualize the retinal pigmented epithelium (RPE) in GA.
- Optical coherence tomography (OCT)
- Multifocal electroretinography
An emerging diagnostic tool your retina specialist may use is Optical Coherence Tomography Angiography (OCTA), which is used to examine the vasculature of the retina..
The Importance of Early Diagnosis
An important point to understand is that geographic atrophy lesions outside the fovea (your central vision) grow more quickly than those in the fovea, meaning it’s important to start treatment before it affects your central vision GA treatments are now available (see below), so dry AMD patients should have a discussion with their general ophthalmologist or retina specialist about where they are in the progression of their condition. If dry AMD advances to geographic atrophy, early intervention offers your best chance to preserve useful sight.
Geographic Atrophy Treatment
As of 2023, two new medications were approved by the FDA for the treatment of Geographic Atrophy: Syfovre, and Izervay.
Neither Syfovre or Izervay are a treatment for early dry AMD, and will not completely halt disease progression like anti-VEGFs do for wet AMD.
Syfovre
Syfovre™ (pegcetacoplan) is administered monthly, or every other month, by injection into the eye, and works by targeting a protein in the complement system known as C3. The complement system is part of the body’s immune system, and protects the body from infection while removing foreign material. C3 activates the complement system.
In clinical trials, Syfovre™ was studied in over 1200 people who had lesions in the center of their macula as well as those who did not. Syfovre™ was shown to reduce the rate of GA lesion growth by up to 42% with monthly injections in people without lesions in the center of the macula from Year 2 to the end of Year 3.
Also see the SYFOVRE safety information page.
Izervay
Izervay (avacincaptad pegol) is another treatment option for GA, and is given as an eye injection once a month, for up to 12 months.
Izervay works by blocking excess production of the C5 protein, part of the immune system’s early response system, which researchers believe causes the development of GA lesions and scarring that cause vision loss.
Clinical trials of Izervay showed a reduction in the rate of GA lesion growth by about 35%.See also: Izervay safety information page
Associated Risks of Treatment
Syfovre and Izervay, and other GA treatments that may follow it, represent a new frontier in macular degeneration treatment. As with other treatments for eye conditions, there are slight risks in using both drugs, and patients should speak with their doctors about those risks, which include:
- A slightly elevated risk for developing wet AMD
- Other rare inflammatory eye complications that accompany an injection into the eye (rare cases of occlusive retinal vasculitis have been reported in .01% or 1 in 10,000 injections)
Sources
- Saundankar V, Borns M, Broderick K, et al. Annual prevalence of geographic atrophy and wet age-related macular degeneration among Medicare Advantage enrollees in a US health plan. J 1 Manag Care Spec Pharm. 2025;31(1):88-94. doi:10.18553/jmcp.2025.31.1.88 https://www.jmcp.org/doi/10.18553/jmcp.2025.31.1.88
- Jaffe, G. J., Westby, K., & Csaky, K. G. (2023). Geographic atrophy: Mechanism of disease, pathophysiology, and role of the complement system. Progress in Retinal and Eye Research, 88, 101046. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10408405/ Accessed 11 March 2025.
- Armento A, Ueffing M, Clark SJ. The complement system in age-related macular degeneration. Cell Mol Life Sci. 2021 May;78(10):4487-4505. doi: 10.1007/s00018-021-03796-9. Epub 2021 Mar 9. PMID: 33751148; PMCID: PMC8195907.https://pmc.ncbi.nlm.nih.gov/articles/PMC8195907/
- Song D, Hua P, VanderBeek BL, Dunaief JL, Grunwald JE, Daniel E, Maguire MG, Martin DF, Ying GS; CATT Research Group. SYSTEMIC MEDICATION USE AND THE INCIDENCE AND GROWTH OF GEOGRAPHIC ATROPHY IN THE COMPARISON OF AGE-RELATED MACULAR DEGENERATION TREATMENTS TRIALS. Retina. 2021 Jul 1;41(7):1455-1462. doi: 10.1097/IAE.0000000000003075. PMID: 33332813; PMCID: PMC9296271.https://pmc.ncbi.nlm.nih.gov/articles/PMC9296271
- Nielsen, M. K., Shah, Y. S., Do, D. V., Bhagat, N., & Lim, J. (2021, December 18). Geographic atrophy. EyeWiki. Retrieved February 20, 2023, from https://eyewiki.aao.org/Geographic_Atrophy
- U.S. Department of Health and Human Services. (2023, December 12). Story of discovery: Nei-funded research paves way for New Dry Amd Drugs. National Eye Institute. https://www.nei.nih.gov/about/news-and-events/news/story-discovery-nei-funded-research-paves-way-new-dry-amd-drugs
- “U.S. FDA Approves Expanded Label for Astellas’ IZERVAY™ (avacincaptad pegol intravitreal solution) for Geographic Atrophy.” Astellas Pharma Inc., 13 Feb. 2025, https://www.astellas.com/en/news/29641. Accessed 11 March 2025.
Was this helpful?
You can support bringing this kind of helpful information to the public. All of our educational materials, including this website, are made possible by individual donor support. Your donation, today, supports our work and allows us to continue providing free information and resources to people with macular degeneration.

